Cox Proportional Hazards Models: Exploring Reproductive Milestones and Mortality in Women
Introduction
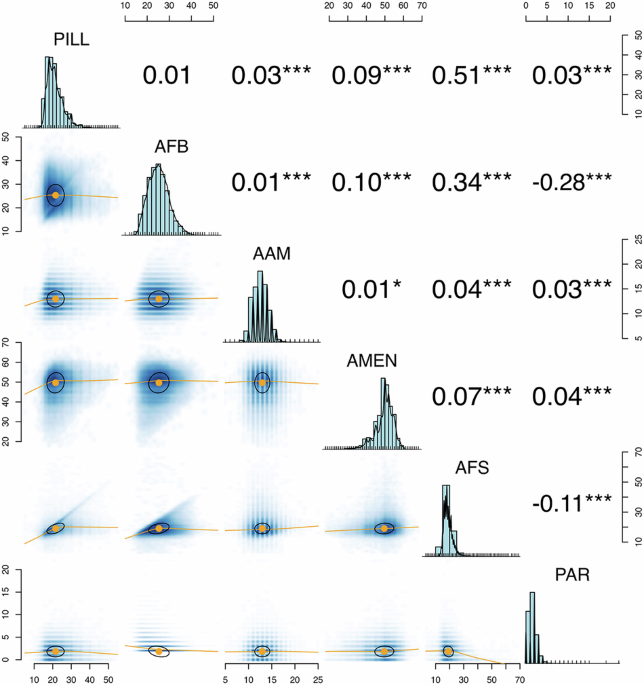
Research utilizing Cox proportional hazards models has highlighted the significant role of reproductive milestones in predicting mortality rates among women in the UK. Central to this study are various milestones, including the onset of oral contraceptive use, age at menarche, age at first sexual intercourse, age at first birth, age at menopause, and total parity, which emerged as influential predictors of long-term survival.
Significance of Reproductive Milestones
The findings indicate that reproductive milestones are comparable, if not more influential, than socioeconomic factors such as education and income regarding mortality prediction. Notably, the impact of these milestones remained significant for up to five decades, emphasizing the importance of recalling reproductive history accurately.
Data Collection and Accuracy
Utilizing data from the UK Biobank, individuals provided repeated reports on reproductive milestones over several years. This method allowed for precise measurement of test-retest accuracy and analysis of recall biases. The accuracy varied by milestone: while the age at menopause showed a recall accuracy of 43%, total parity boasted 99.2% accuracy, indicating the robustness of self-reported data.
Predictive Capacity in Mortality Models
In total, 8,116 deaths were classified according to the International Classification of Diseases (ICD-10). The Cox proportional hazards models revealed noteworthy associations between reproductive milestones and mortality risk. For example, age at first birth was strongly linked to post-reproductive mortality risk. Specifically, each additional year at first birth was associated with lower mortality risk, independent of various socio-economic factors.
Effects of Oral Contraceptive Timing
Oral contraceptive use emerged as a major predictor of mortality risk, with significant effects observed even decades post-use. This result transcended other analyzed variables, maintaining its significance even within stratified age groups. However, the timing of contraceptive use was the only variable that deviated from expected z-test outcomes for proportional hazards, suggesting the influence of changing formulations and types of oral contraceptives over time.
Influence of Menarche and Menopause
Both age at menarche and age at menopause were examined as mortality predictors, indicating that later onset correlates with increased all-cause mortality risk. Specifically, each year of delay in menarche reportedly increases mortality risk by approximately 3.5%, while menopause delay predicts an increase of 1.4%. These findings contribute essential knowledge towards understanding public health impacts concerning reproductive health timing.
Nonlinear Relationships and Complex Interactions
The analysis of nonlinear interactions revealed that while simple linear models provided significant regression results, they often masked more intricate relationships. For instance, age at menarche displayed a U-shaped pattern in mortality risk, adding depth to the understanding of reproductive timing and overall health outcomes.
Implications for Future Research
The research underscores the multifaceted relationships between reproductive milestones and health outcomes. It remains crucial for future studies to further explore how these factors interact over time, particularly concerning aging and mortality rates, to ultimately enhance healthcare paradigms for women.
Conclusion
This body of research significantly enriches the understanding of reproductive history’s relevance to women’s health outcomes in later life. Through robust statistical modeling and rigorous data collection, it invites a closer examination of the intersections between reproductive choices and mortality risks, with important implications for public health policies and women’s health initiatives.
References
The original study data, including figures and tables, can be further explored through the publication in relevant journals.