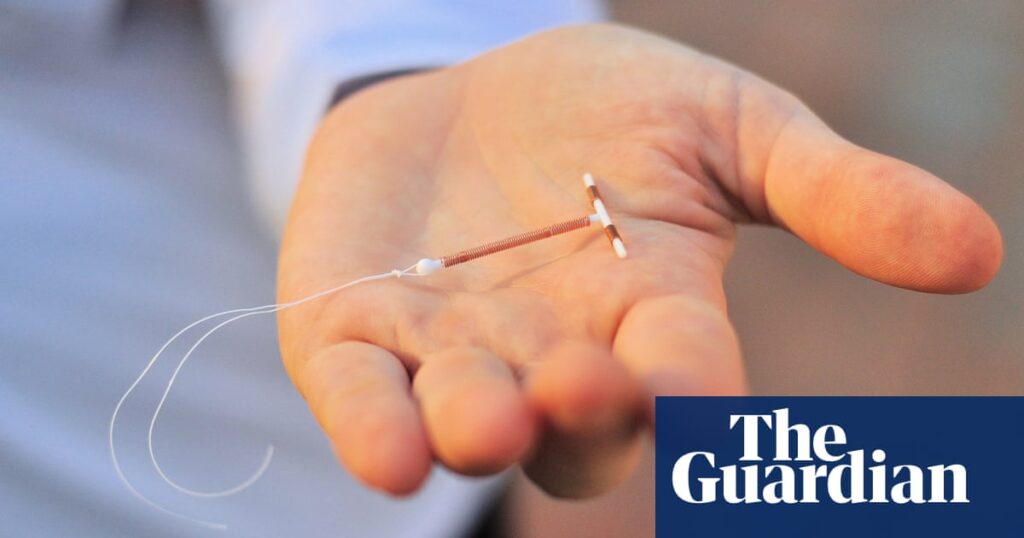
Understanding the Low Uptake of IUDs Among Australian Women
Intrauterine devices (IUDs) are recognized as one of the most effective forms of contraception available, yet awareness among Australian women remains alarmingly low. A recent survey conducted by Jean Hailes has highlighted this gap in public education, attributing it to the relatively minimal adoption of IUDs in comparison to other Western countries.
Survey Findings
The Jean Hailes National Women’s Health Survey, which included responses from 3,537 reproductive-age women, revealed that although over 80% of women aged 18 to 24 and 60% of those aged 25 to 44 expressed a desire to avoid pregnancy, the use of IUDs was minimal. Only:
- 7% of women aged 18-24
- 11% of women aged 25-44
reported using an IUD as their chosen contraceptive method.
Comparative Usage Rates
Dr. Sarah White, CEO of Jean Hailes, noted that Australia significantly lags behind other countries such as the UK, South Korea, France, and the US, where IUD usage rates exceed 30%. This discrepancy raises concerns about the effectiveness of existing public health education initiatives.
The Efficiency of IUDs
IUDs are small devices inserted into the uterus, providing over 99% efficacy in preventing pregnancies, especially when compared to contraceptive pills, which, while also highly effective, can be influenced by irregular usage and other factors like gastrointestinal disturbances.
Misconceptions and Knowledge Gaps
The survey further indicated that many women misunderstood the effectiveness of different contraceptive methods:
- 32% incorrectly identified condoms as the most effective method.
- 27% thought all methods were equally effective.
- Only 27% recognized IUDs as the most effective option.
Dr. White emphasized that this lack of awareness drives low IUD uptake, with many women unknowingly overlooking an optimal contraceptive option.
Unplanned Pregnancies
The survey highlighted that 30% of women aged 25 to 44 and 8% of those aged 18 to 24 reported experiencing unplanned pregnancies, underscoring the urgent need for improved education about these contraceptive alternatives.
Barriers to Awareness and Access
Professor Danielle Mazza, a leader in women’s sexual and reproductive health research, pointed out that inadequate training for healthcare providers in IUD insertion contributes to the low rate of prescription and the subsequent lack of emphasis on their benefits. In response, the federal government has increased reimbursements for IUD services and is set to introduce training centers aimed at enhancing healthcare provider competencies.
Additionally, while IUDs present higher initial costs when sourced via private providers, they often provide greater long-term cost efficiency compared to contraceptive pills and condoms.
Perceptions of Pain and Insertion
Concerns about discomfort during insertion, often magnified by negative social media narratives, deter many women from considering IUDs. However, experience suggests that many patients report the procedure is less painful than anticipated.
The Path Forward
As states transition to pharmacy prescription models for contraceptive pills, it is essential that women receive comprehensive guidance on all contraceptive options, including long-acting reversible contraceptives (LARCs) like IUDs. Public education initiatives focused on the effectiveness and convenience of IUDs could significantly shift perceptions and increase usage rates.
Dr. White concluded that improved accessibility and education in rural and regional areas could enable more women to consider IUDs as a viable contraceptive option, ultimately enhancing reproductive health outcomes across Australia.