In regions characterized by limited medical resources, particularly high-burden areas like rural China, raising awareness about HPV and its vaccination is foundational for cervical cancer prevention. This is especially crucial where around 60% of cervical cancer cases occur amid low screening participation and awareness.
Our extensive study involving 8,618 participants investigates the level of HPV awareness, willingness to receive the vaccine, and the systemic obstacles faced by this underserved population. Given the global relevance of our findings, they offer significant insights applicable to various high-cervical cancer burden populations worldwide.
Current Awareness and Educational Gaps
Despite advancements through health initiatives, specific awareness of HPV remains alarmingly low. Our research found that only 30.0% of participants were aware of HPV, and 35.4% knew about the HPV vaccine. These figures are considerably lower than those reported in urban China (60.75%) and Western countries (61.6% to 87.7%). Notably, longitudinal data indicates a positive trend; HPV awareness has risen from a mere 0.14% in 2008, highlighting the effectiveness of government-funded screening programs and targeted health education campaigns in regions like Xinjiang.
Vaccination Rates and Willingness
An alarming finding from our study is the extremely low HPV vaccination rate of just 1.1%. National data from the China CDC Weekly shows significant disparities in vaccine coverage among females aged 9-45. First-dose coverage sits at 10.15%, dwindling to 8.69% for the second dose and 6.21% for the third. Regions such as Beijing and Shanghai display higher vaccination rates (25.40% and 20.99%, respectively), while Xinjiang and Qinghai lag behind at below 5%. Importantly, our study indicates that 91.3% of married women expressed a willingness to vaccinate themselves, and 85.3% showed intent to vaccinate their daughters upon learning about the vaccine’s benefits, indicating a significant opportunity for increasing uptake through enhanced awareness.
Correlates of Vaccination Intent
In exploring factors influencing vaccination decisions, our study uncovered a divergence compared to global trends: willingness to self-vaccinate is poorly correlated with awareness of HPV and its vaccine. This suggests that maternal resolve, rather than mere knowledge, plays a pivotal role in intergenerational vaccine decisions among rural women. Age and marital status emerged as influential factors. Interestingly, younger mothers (under 35 years) often perceived their daughters as “too young” for vaccination, and single mothers exhibited a significantly lower intent to vaccinate, likely due to financial concerns or misconceptions regarding HPV transmission.
Socioeconomic Determinants and Cultural Barriers
Socioeconomic factors such as education and occupation have been shown to impact HPV awareness significantly. In Xinjiang, the intersection of these disparities is particularly stark due to its diverse demographic composition. Our findings underscore the urgent need for culturally tailored interventions, including educational initiatives aimed at illiterate elderly farmers, to enhance cervical cancer screening participation and HPV knowledge.
Cervical Cancer Screening Challenges
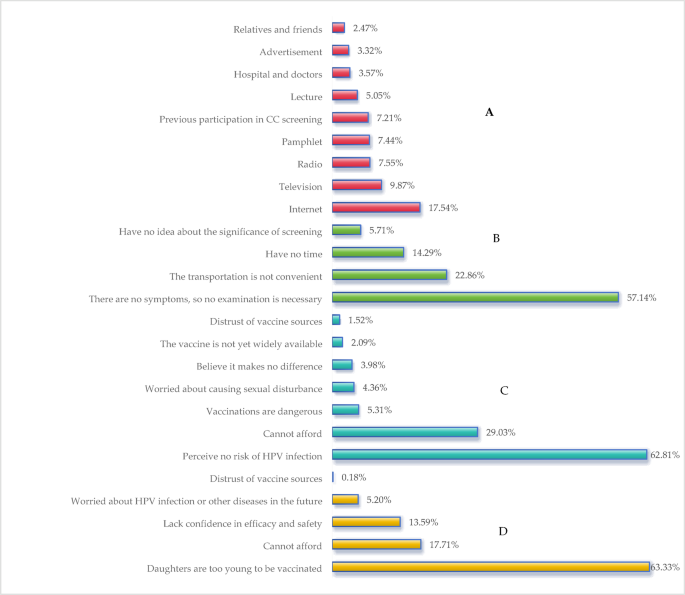
Despite initiatives like the National Cervical Cancer Screening Program (NCCSP) aiming to screen 10 million rural women annually, implementation has fallen short. Our study found that only 19.9% of participants engaged in cervical cancer screening, significantly lower than the national average of 36.8%. Alarmingly, only 80.61% of women with cervical abnormalities received necessary treatment, failing to meet the WHO’s targeted 90% treatment goal. The barriers identified in our research—primarily the perception of having “no symptoms”—obscure the necessity of routine screenings, as highlighted in a systematic review identifying common barriers such as embarrassment or fear associated with medical procedures.
Misconceptions Affecting Vaccination Acceptance
Our study also revealed misconceptions surrounding HPV vaccination, including the belief that the risk of HPV infection is low and that daughters are too young for vaccination. This underlines a significant disconnect, as those with lower awareness may lack understanding of the vaccine’s efficacy, detracting from considerations of cost and necessity.
Information Sources and Media Influence
Participants primarily obtained information about cervical cancer and HPV vaccines from the Internet, television, and past screening activities. While globally, social media plays an increasing role in disseminating health information, in our study, rural women predominantly relied on traditional media. Young individuals tend to navigate new media effectively, suggesting an opportunity for health communication initiatives via popular platforms like WeChat and TikTok, which could enhance HPV education and encourage vaccination interactions.
Study Limitations
While our study has a substantial sample size, it primarily reflects the experiences of rural women in southern Xinjiang. Exclusions based on menstruation, pregnancy, or refusal of screening may introduce selection bias, and reliance on self-reported medical history can yield inaccuracies. Cultural stigmas related to STI discussions may affect the validity of collected data. Although standardized training was provided to interviewers to mitigate potential biases, further comprehensive studies are needed to introduce psychometric validation. Additionally, our study did not explore economic factors influencing HPV vaccination uptake, highlighting a potential area for future research.